New study suggests immune cells may explain why chronic pain lasts longer in women
Findings could lead to new treatment options in the future
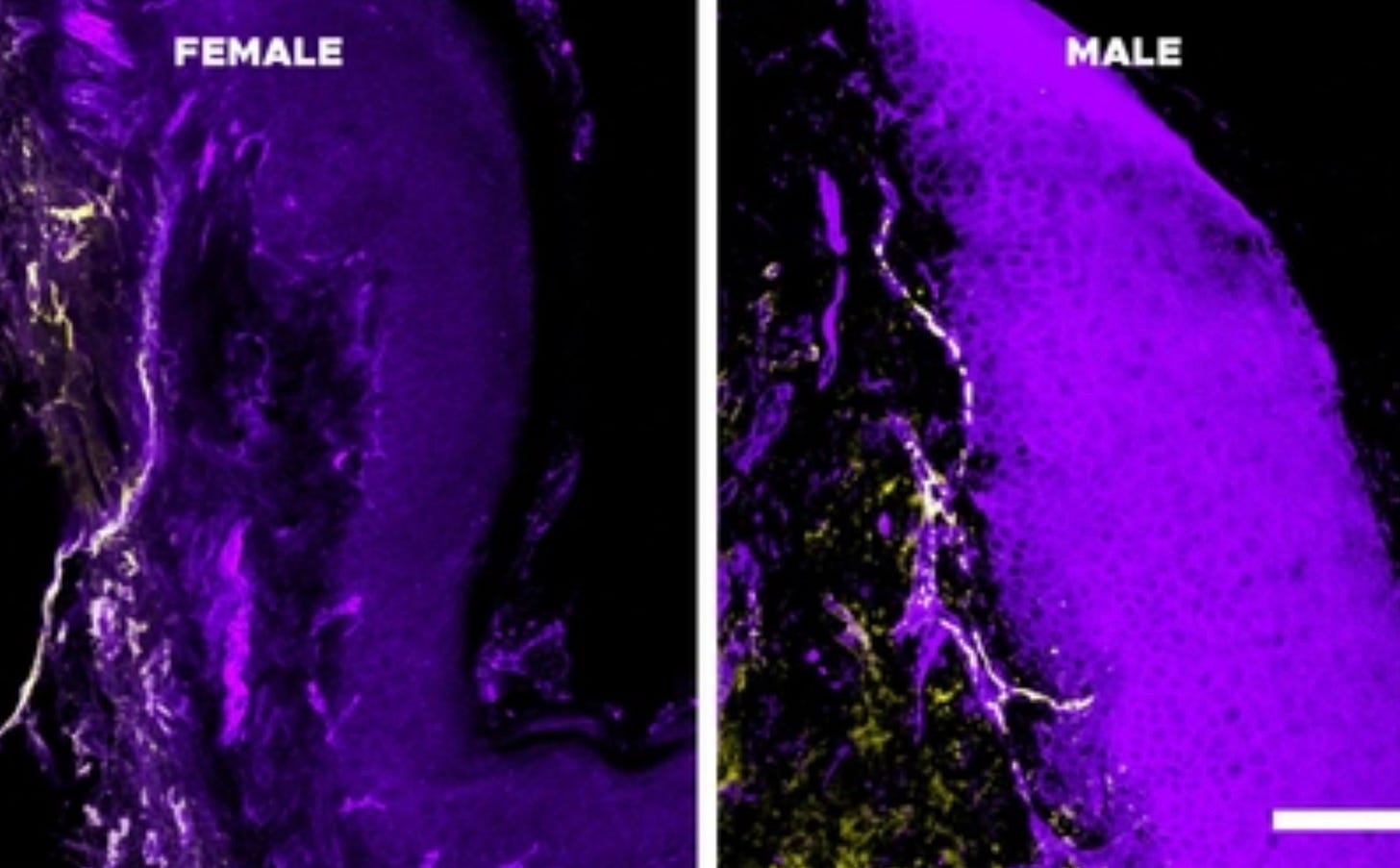
Chronic pain is one of the most common reasons women seek medical care, yet it remains poorly understood — and often lasts longer in women than in men. Now new research suggests the immune system may help explain why.
In a study published in Science Immunology, researchers at Michigan State University found that certain immune cells play an important role in switching off pain once an injury or illness has passed. The findings suggest that differences in how these cells behave in men and women may contribute to longer-lasting pain in women.
The researchers focused on a type of immune cell called a monocyte, which produces a molecule known as interleukin-10 (IL-10). This molecule helps reduce inflammation and signals to pain-sensing nerves that it is time to shut down the pain response. The team found that IL-10-producing monocytes were more active in males, partly due to the influence of sex hormones such as testosterone, while females showed lower activity and slower recovery from pain. The same pattern was observed in both laboratory models and human patients.
“The difference in pain between men and women has a biological basis,” said Geoffroy Laumet, associate professor of physiology at Michigan State University and lead researcher on the study.
“It’s not in your head, and you’re not soft. It’s in your immune system.”
The findings challenge the traditional view that the immune system mainly contributes to pain by causing inflammation. Instead, the study suggests that resolving pain is an active biological process driven by immune signals.
“This study shows that pain resolution is not a passive process,” Laumet said. “It is an active, immune-driven one.”
Around 50 million Americans live with chronic pain, with women disproportionately affected. Researchers say the biological mechanisms behind these sex differences have historically been poorly understood.
By identifying immune pathways involved in pain resolution, the study points to possible future treatments that could help the body switch off pain more effectively. Researchers say therapies that increase IL-10 activity could eventually offer new non-opioid approaches to chronic pain treatment.
“Future researchers can build on this work,” Laumet said. “This opens new avenues for non-opioid therapies aimed at preventing chronic pain before it’s established.”
While treatments based on these findings are likely years away, the research provides new evidence that sex differences in pain are rooted in biology — and could help guide the development of more effective treatments.
You might also like:



I’m a immune deficiency person with chronic pain I use Cbd oil for pain relief and I get ivigg monthly for Cvid seems with all this I still have pain just not as bad as long as I use Cbd oil ! The igg helps my mold allergy symptoms the worst is the mucus discharge I get